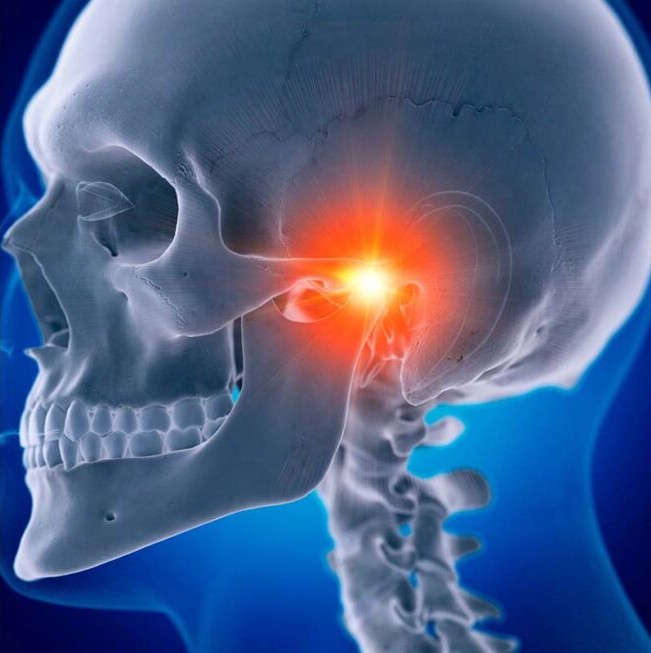
The TMJ or otherwise known as the Temporomandibular Joint, is a very common problem for many people. From jaw popping with or without pain, grinding when under stress or sleeping, limited jaw opening distance or even locking of the jaw. I have seen many patients with the above issue and I treat most of them with the same protocol once properly diagnosed. Dentists can be very helpful in not only diagnosing TMJ Disorder or TMD as the Mayo Clinic labels it, but they can help treat by creating a bite guard or plate that is to be worn mostly when sleeping (since that’s where most of the clenching or grinding takes place). Dentists can also refer to TMJ Specialists who are typically dentists with additional training in TMD and Sleep Medicine.
The TMJ name comes from the relationship between the Temporal bone (side of the skull, where the ear is located) and Mandible bone (lower jaw) of the skull. There is a small disc where the two bones meet but it isn’t like the disc in the spine. The TMJ disc (or articular disc) is a small, biconcave (dips in on both sides) piece of dense fibrous connection tissue located within the TMJ, which connects the jaw to the skull. Acting as a shock absorber and cushion, it separates the joint into superior and inferior (top and bottom) compartments to ensure smooth jaw movement during activities like chewing and speaking. There are four muscles involved with the movement of the TMJ – Masseter, Temporalis, Medial Pterygoid and Lateral Pterygoid.
When I was in Chiropractic school at National University of Health Sciences in Lombard, Illinois, there was not only anatomy classes and dissection labs using cadavers, but also motion palpation and treatment labs where we were taught how to diagnosis TMD. Once we understood the anatomy, physiology and mechanics of the TMJ we used an assessment guideline to find the source of the problem.
There is a large contribution of soft tissue or muscle involved with TMD. There are Chiropractic adjustments for the TMJ but in my Chiropractic practice, that is the last resort. I typically observe the movement of the jaw by assessing for either muscular or capsular (joint capsule) involvement by watching the movement pattern. Muscular involvement is a better option than capsular involvement. Capsular involvement is a chronic muscular problem. Both the muscular and capsular involvement can create joint malalignment and restriction in movement. Even with the joint malalignment and restrictions, I prefer to address either the muscular and capsular involvement with home Isometric exercises being taught and soft tissue techniques like extraoral (outside of the mouth) myofascial release on the Masseter and Temporalis muscles. I personally use a specialized device called the Rapid Release (www.rapidreleasetech.com) that uses a vibration frequency to disturb chronically tight muscle and capsular tissue. In addition to the use of the Rapid Release device, I also do Chiropractic adjustments to the Cervical (neck) and Thoracic (mid back) spine which are contributing areas to the soft tissues that connect and contribute to the overall mechanics of the TMJ like the SCM (Sternocleidomastoid) muscles, Scalene muscles, Trapezius muscles, Levator Scapulae muscles, and paraspinal muscles. Often, these Cervical and Thoracic spine muscles are also addressed with the Rapid Release device.
Since the scope of practice for Chiropractic in Washington State doesn’t allow for intraoral (inside of the mouth) myofascial release, I would suggest a couple different options here. First option, I have professional relationships with Licensed Massage Therapists who are certified in the treatment of TMD and can perform intraoral myofascial techniques. Second option, I give patients the names of the two intraoral muscles needing to be addressed and ask them to look up the myofascial techniques and instruction to get to the Lateral Pterygoid and Temporalis muscles themselves.
Once the above treatment plan is used for 4-12 visits and I can see how beneficial it was, this would be when I consider Chiropractic adjusting to the TMJ. The Chiropractic adjustment can look intense and aggressive but really, it’s a slight movement along the plane or angle of the Mandible. The side of the TMJ along with the amount of force needed is determined by motion palpation techniques.
The combination of myofascial techniques, Isometric home exercises, bite guard, stress management, and Chiropractic adjusting (if needed) have proven to be very effective in my practice for the treatment of TMD.
Thanks for reading – stay well.
Dr. SJ
